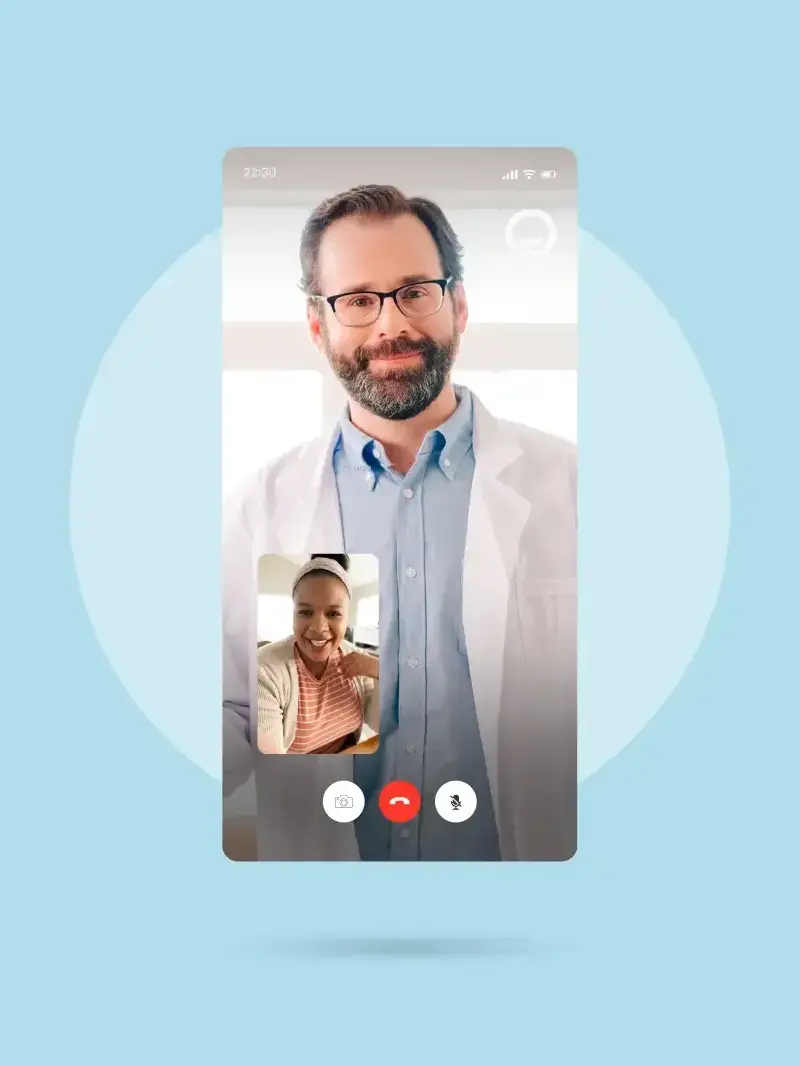
COVID evaluation available online
If you are experiencing COVID-19 symptoms, had close exposure to someone diagnosed with COVID-19, or have tested positive at home, consult with one of our board-certified primary care doctors online today to discuss the management of symptoms, prescribe medications if appropriate, and provide work/school excuse notes during the time of your illness. Our top-rated primary care doctors can evaluate symptoms and prescribe cough suppressants and breathing treatments to reduce your symptoms. For people at high risk of complications from COVID-19, antiviral medication may be appropriate to reduce the risk of your infection progressing to severe illness.*
*Prescriptions are provided at the doctor’s discretion. You may qualify for antiviral therapy if you are: within 5 days of experiencing mild to moderate COVID symptoms, confirmed to be COVID-19 positive via PCR or rapid antigen test, and are at high risk of complications from COVID-19 infection. Learn more about our controlled substances policy and our prescription discount card.
COVID treatment services
The COVID-19 virus has changed over time. These changes, or mutations, are referred to as variants since they vary from the original virus. COVID-19 variants identified as being monitored by the World Health Organization include the Omicron (including the newly emerging JN.1 variant). Older variants including Delta, Gamma, Beta, and Alpha strains are rarely seen in the United States at this time, and changes in the circulating variants are to be expected.
With access to PlushCare's COVID care online, you can meet with a top board-certified primary care doctor via an online consultation. Our doctors can help you interpret your home COVID testing results, discuss home care options, and prescribe the appropriate COVID medication that can help manage symptoms, and when appropriate prescribe oral antiviral treatment. If you are seen while you are sick, our doctors can provide work/school excuse notes so you can recover at home. Our doctors can not provide work notes if you come to us after your illness.
Our treatment options and offerings include:
COVID testing
The difference between a COVID-19 diagnostic test and antibody test is that a diagnostic test is performed to determine if a person currently tests positive or negative for COVID-19, while an antibody test is used to find out if a person had a COVID-19 infection in the past.
While a COVID-19 diagnostic test is for people who may be experiencing symptoms of a current illness, an antibody test is for people whose symptoms have subsided for at least 10 days. A doctor’s order may be required for an antibody test, which requires blood to be taken.
Diagnostic tests typically require a nasal swab, throat swab, or saliva sample. Tests can either be performed in a medical setting, or via COVID-19 at-home test kit. While PCR tests are typically considered more reliable than antigen tests, any individual test may or may not be accurate; additional testing may be required in order to verify results. If either test is positive, then it’s likely that the person has a current COVID infection. If a test is negative, then it may be correct or it may be a false negative result. Talk to one of our online doctors today to help interpret your test results.
How to get a COVID-19 antibody test
You can get COVID-19 antibody testing by visiting a lab center, where the blood test will be performed. There is also an option to receive an at home test in the mail that you have to ship back for the test to be completed. Note that a physician’s order or referral may be required before COVID-19 serology/antibody testing can be performed. One of our board-certified primary care doctors may be able to provide you with a testing order for a COVID-19 antibody test following an evaluation online.
COVID vaccine
The three COVID-19 vaccines available in the United States are the Pfizer-BioNTech vaccine, Moderna vaccine, and Novavax vaccine. Both the Pfizer and Moderna vaccines are FDA approved for people 6 months and older, and the Novavax vaccine is available for individuals aged 12 years or older and is approved under the Emergency Use Authorization (EUA) Act.
The Moderna and Pfizer vaccines are mRNA vaccines The newest option, Novavax, is a monovalent recombinant protein vaccine and does not contain RNA particles. The Johnson & Johnson COVID-19 vaccine is no longer available in the United States.
Possible COVID-19 vaccine side effects may include:
-
Pain, swelling, or redness at the injection site
-
Swollen lymph nodes in the armpit
-
Joint or muscle pain
-
Headache
-
Tiredness
-
Nausea and vomiting
-
Fever and chills
-
Myocarditis or pericarditis (very rare)
-
Anaphylaxis (extremely rare)
Side effects after vaccination should go away in a few days. Most people experience no side effects. The coronavirus vaccines are generally considered safe, and allergic reactions are rare. Everyone who receives a COVID-19 vaccine should be monitored for 15 minutes by medical personnel after the vaccine is administered.
A COVID-19 vaccine card is usually provided tovaccine recipients, which serves as a record to keep track of vaccination information.
COVID-19 Booster
If you have questions about booster shots, you can book an appointment with one of our primary care doctors online to discuss if a booster shot is appropriate. These recommendations are changing as more information becomes available; you can also check the CDC website prior to scheduling your booster shot for updated information.
COVID medication
COVID-19 medications include Pfizer’s Paxlovid (nirmatrelvir/ritonavir) and Merck’s Lagevrio (molnupiravir). At this time, Paxlovid is approved by the FDA for use in people with mild to moderate COVID who are at high risk of complications from the infection. Lagevrio is approved under the emergency use authorization (EUA) Act from the FDA for the same indication as Paxlovid. COVID-19 medication can help prevent severe illness in high-risk patients to help keep them out of the hospital. These medications are not helpful for people with COVID infection who are at low risk of complications and are not helpful for anyone who is beyond five days from onset of their symptoms.
These antiviral medications are for people who have recently experienced mild to moderate COVID-19 symptoms and are considered part of high-risk groups. These pills can reduce the risk of the illness progressing to severe disease, leading to hospitalization, respiratory failure, and even death
-
The Pfizer COVID medication, Paxlovid, is three pills taken twice daily for 5 days and must be started within 5 days of onset of COVID symptoms. Each carton contains 30 tablets divided in 5 daily-dose blister cards. If you have chronic kidney disease, it is important to discuss this with your doctor, who may recommend a lower dose of Paxlovid for you.
-
The Merck COVID medication, Lagevrio, is four capsules taken twice a day for 5 days. Similar to Paxlovid, it is also intended to be started within 5 days of the onset of mild to moderate COVID symptoms and is only intended for people at high risk of complications from COVID. Lagevrio does not require dose adjustment for people with chronic kidney disease and has fewer potential medication interactions than Paxlovid.
There are no oral medications designed to be taken at home for people with severe COVID illness, including great difficulty breathing, persistent high fever, or persistent low oxygen levels. People with severe COVID are best cared for in a hospital.
The COVID-19 oral medications works by disrupting the function of the SARS-CoV-2 virus. The Pfizer COVID-19 pill works by blocking a step in the SARS-CoV-2 replication process, preventing viral RNA from replicating. The Merck COVID-19 pill creates mutations in the coronavirus’s genetic code while it replicates; eventually, the coronavirus will have too many mutations to function, causing the virus to die.
Side effects of the COVID-19 pills depend on the specific medication. Paxlovid in particular has a significant number of drug interactions between it and other common medications. This is one reason why it’s important to have a thorough discussion with your physician about your medical history and all current medications you are taking if you are considering a prescription for COVID pills.
The current supply of both oral COVID treatments is pretty good in local pharmacies, but it is difficult for your doctor to know if your insurance will cover the full cost of your medication. Patients are advised to call or go online to their insurance company’s website to check this.
Due to a lack of scientific data at this time, PlushCare physicians do not prescribe ivermectin, hydroxychloroquine, or azithromycin/other antibiotics to treat COVID-19.
COVID symptoms
According to the Centers for Disease Control and Prevention (CDC), COVID-19 symptoms may include:
-
Fever or chills
-
Cough
-
Shortness of breath
-
Muscle or body aches
-
Fatigue
-
New loss of taste and smell
-
Headache
-
Sore throat
-
Congestion or runny nose
-
Pink eye
-
Nausea
-
Vomiting
-
Diarrhea
This does not include all possible symptoms. COVID-19 symptoms can range from mild to severe. If someone experiences any of the emergency warning signs of COVID-19, they should get emergency medication attention immediately. These serious symptoms may include: difficulty breathing, inability to wake or stay awake, chest pain, or pale, gray, or blue-colored skin or lips.
It is important to note that COVID has some of the same symptoms as the flu, common cold, allergies and sinusitis. The only way to confirm a COVID-19 diagnosis is by taking a COVID-19 test.
Over the years COVID symptoms have changed, and it is less common to experience severe fatigue, loss of smell or taste or high fever. COVID can look like any other common cold or flu bug, or even like mild allergy symptoms, which is one reason why it persists. Many people don’t realize that their annual sinusitis or bronchitis is caused by COVID this year. For this reason, our doctors always recommend an at-home COVID test if there are any signs of an upper respiratory infection.
COVID in children
COVID-19 can affect people of all age groups, including children. Children are also at risk of contracting mild to severe COVID-19 illness. While COVID-19 symptoms in children typically appear in a milder and more cold-like form than in adults, there is still a potential for long-term COVID effects in children. Children are also more likely than adults to develop pink eye (conjunctivitis) with their COVID infection.
Long-term effects of COVID-19
Some people may experience long COVID, also called long-haul COVID, which means having COVID-19 symptoms or related health problems for more than one month after initially recovering from a COVID illness. The long-term effects of COVID-19 can vary, and are still being studied in clinical trials in order to better understand them.
Possible long-term effects or symptoms after initially recovering from the coronavirus disease may include:
-
Fatigue
-
Cough
-
Shortness of breath
-
Joint pain
-
Chest pain
-
Difficulty concentrating
-
Rapid heartbeat
-
Headaches
-
Depression or anxiety
-
Loss of taste or smell
-
Intermittent fever
Mental health struggles after moderate and severe cases of COVID-19 can be especially challenging for patients who were hospitalized.
A rare yet serious COVID complication which may affect people, primarily children, is multisystem inflammatory syndrome. This causes inflammation in different areas of the body and may potentially lead to severe heart damage, requiring special care from a pediatric cardiologist.
Some larger hospital systems have developed special clinics to support people recovering from long-haul COVID.
While complications of COVID-19 are still being investigated, healthcare providers can help to treat long-term COVID effects by examining each specific symptom. Treatments that may be able to help with ongoing care and recovery include breathing exercises, medications to help reduce symptoms, and specialized physical therapy.
Our board-certified primary care physicians can help discuss your long COVID symptoms and discuss potential treatments. Often, in-person evaluation is required to accurately evaluate symptoms, and our doctors can help provide referrals to appropriate specialist care when needed. Our doctors are rarely able to establish a new diagnosis of long COVID or provide disability determination through online evaluation.
COVID treatment FAQs
When should I start treatment for COVID-19?
Contact a doctor immediately if you have serious COVID-19 symptoms. COVID-19 medication can only be started in the first five days from when symptoms begin. If you test positive for COVID-19, speak with one of our board-certified primary care doctors online as soon as possible to see if you qualify for prescription COVID medication. Our doctors can also discuss home care suggestions and provide a note for school or work while you are sick. Our doctors cannot provide notes to cover time away for an illness after the fact, so please schedule your visit while you are sick.
What are some easy ways to protect myself from COVID-19?
If you do not have access to soap and water, you can use hand sanitizer that has at least 60% alcohol.
Wear a mask when traveling in closely packed spaces such as an airplane or train.
Get vaccinated and stay current with COVID boosters.
Should I get the COVID-19 antibody test?
If you experienced COVID-19 symptoms more than 10 days ago, you are eligible for COVID-19 antibody testing. The test will determine if you were exposed to COVID-19 and may indicate immunity for possibly as long as eight months from the time of the test, although more recent research suggests that immunity may drop sooner than that. There is no longer thought to be much benefit to this test as far as predicting current or future immunity to COVID or determining return to work or other decisions. It is becoming less common to order this test, and it is not always covered by insurance. You can schedule an appointment today to discuss with your online doctor if a COVID antibody test is right for you.
What if my COVID-19 antibody test result is positive?
A positive test means you have had the virus in the past, at least two weeks prior to the test, and that your body has antibodies to the virus. Studies show that a positive antibody test means you have some protection against getting a new COVID infection, but that immunity drops quickly between 6-8 months from prior COVID illness or exposure. The antibody test is not able to determine if you have immunity following prior COVID vaccination.
How long does it take to recover from COVID-19?
There are also cases of COVID that can last months. This is sometimes called long haul COVID, or long COVID-19. Patients known as “long haulers” can continue having COVID symptoms for months or years after first getting COVID. This can happen to anyone, no matter their age, health, or severity of symptoms.
Can PlushCare help with the Coronavirus?
According to the CDC, it is highly recommended that you call your doctor before you head over to the doctor’s office. That's where PlushCare steps in! If you don't have a doctor or your doctor is busy, book an appointment with any of our top primary care physicians and they will be able to answer any questions you have about the virus.
Our doctors are able to prescribe Paxlovid or Lagevrio if you qualify. They can also discuss ways to reduce your symptoms and provide work or school excuse notes while you are home sick.
Want to talk to an online primary care doctor about coronavirus prevention, testing, symptom management and more? Book an online information/screening session.
If you have any further questions please give us a call at (800) 221-5140 or email us at info@plushcare.com.
3 simple steps to get COVID care today

Book a COVID care appointment with a doctor online.

Talk to your doctor about your COVID symptoms.
Pick up a prescription for COVID treatment, if you qualify.
COVID treatment pricing details
To request COVID treatment, join our monthly membership and get discounted visits.
30 days of free membership
- Same-day appointments 7 days a week
- Unlimited messages with your Care Team
- Prescription discount card to save up to 80%
- Exclusive discounts on lab tests
- Free memberships for your family
- Cancel anytime
Paying with insurance
Membership
$19.99
First month free
Visits
Copay
Visit price with insurance
Often the same as an office visit. Most patients with in-network insurance pay $30 or less!
We accept these insurance plans and many more:



Paying without insurance
Membership
$19.99
First month free
Visits
$129
Visit price without insurance
Sources:
PlushCare is dedicated to providing you with accurate and trustworthy health information.
-
CDC (Centers for Disease Control and Prevention): "Treatments for Severe Illness." CDC. Accessed on December 14, 2023, at https://www.cdc.gov/coronavirus/2019-ncov/your-health/treatments-for-severe-illness.html.
-
FDA (U.S. Food and Drug Administration): "Know Your Treatment Options for COVID-19." FDA. Accessed on December 14, 2023, at https://www.fda.gov/consumers/consumer-updates/know-your-treatment-options-covid-19.
-
NIH (National Institutes of Health): "COVID-19 Treatment Guidelines." NIH. Accessed on December 14, 2023, at https://www.covid19treatmentguidelines.nih.gov/
-
Mayo Clinic: "Coronavirus (COVID-19) - Symptoms and Causes." Mayo Clinic. Accessed on December 14, 2023, at https://www.mayoclinic.org/diseases-conditions/coronavirus/symptoms-causes/syc-20479963.
PlushCare content is reviewed by MDs, PhDs, NPs, nutritionists, and other healthcare professionals. Learn more about our editorial standards and meet the medical team. The PlushCare site or any linked materials are not intended and should not be construed as medical advice, nor is the information a substitute for professional medical expertise or treatment.